An Apgar score is a clinical measure of a newborn’s well-being and emergency care needs. All infants should receive the test at 1 and 5 minutes after birth. If a baby receives a low score, their medical team should repeat the test every 5 minutes for 20 minutes.
A low Apgar score may indicate a birth injury or other medical issue. If that issue occurred due to medical negligence, you may have a viable birth injury lawsuit. The legal team at our full-service personal injury law firm can help you understand the legal nuances of your case, including the evidentiary role your child’s Apgar score may play.
What Does an Apgar Score Measure?
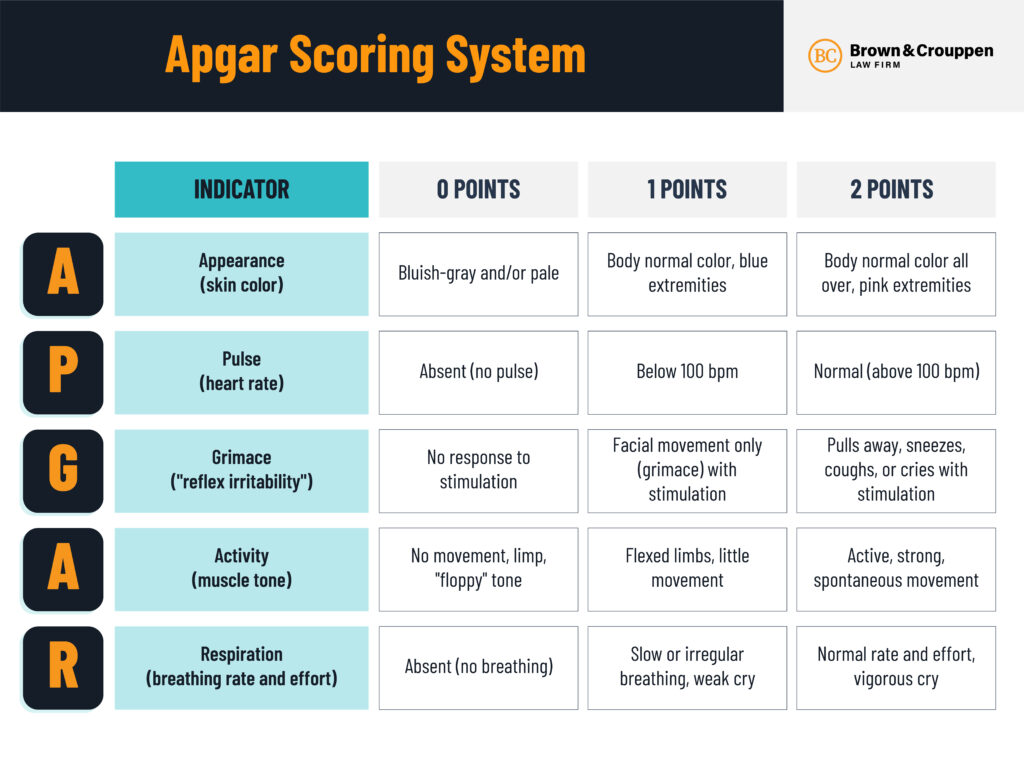
An Apgar score measures a child’s health vitals soon after birth. The Apgar score chart measures five health indicators:
- Appearance – Skin coloration, indicating blood oxygen levels
- Pulse – Heart rate, which should be above 100 beats per minute
- Grimace response – Reflexive reactions to stimulation, facial grimacing serving as a key indicator
- Activity – Spontaneous physical movement
- Respiration – Breath rate and the strength of the newborn’s cry
Babies receive a score of 0, 1, or 2 for each item. A score of 0 indicates a total absence of the sign, and a 2 indicates a strong presence. The total score indicates whether a baby needs additional support or emergency care.
What Is a Normal Apgar Score?
Apgar scoring runs from 0–10, with a normal score falling between 7–10. Very few infants receive a “perfect” 10 because most newborns have blue hands and feet immediately after birth.
For babies born at or close to term, a score of 4–6 at 5 minutes is “moderately abnormal” and may indicate a need for active intervention. Children in this category usually receive follow-up Apgar tests at 10, 15, and 20 minutes post-birth, or until their Apgar score falls within the normal range.
A score of 0–3 is very low. Scores in this range represent a medical emergency that may require resuscitation, which should begin as soon as possible. Waiting too long for an Apgar score to begin resuscitation may amount to medical malpractice.
What Does a Low Apgar Score Indicate?
An Apgar score lower than 7 also needs immediate medical attention. Among other things, it may indicate a need for:
- Supplemental oxygen
- Clearing of any fluid in the baby’s airway
- Physical stimulation to increase the baby’s heart rate
These simple interventions often resolve the problem. Low scores at 1 minute post-birth often normalize by 5 minutes. However, children whose scores remain in the 0–3 range at 5 minutes have a reduced chance of survival and often need admission to the neonatal intensive care unit.
If an infant’s Apgar score remains at 0 for 10 minutes, the likelihood of survival with normal brain function is low. Resuscitation may fail if no heartbeat is detectable at 10 minutes.
A low initial Apgar score does not reliably predict individual long-term outcomes, but the overall risk of neurological disability is higher among children with low Apgar scores at 5 minutes.
For example, newborns with a 5-minute score between 0–3 have an increased risk of developing cerebral palsy. The risk may be between 20–100 times higher in babies with a score between 7–10.


Were you injured in an accident due to someone else’s negligence? Get legal help from the most effective injury law firm in the Midwest.
What Causes a Low Apgar Score?
Lower scores are common following difficult births and when fluids obstruct a newborn’s airway. Other risk factors include:
- Birth at less than 37 weeks or more than 42 weeks gestation
- Birth weight below 5.5 pounds or above 8.8 pounds
- Use of pain medication during delivery
- Presentation in breech position
- Neonatal feces, also called meconium, in the amniotic fluid
- C-sections when three or more minutes pass from incision to delivery
- C-sections under general anesthesia
- Induction of labor using oxytocin
Many of these risk factors are preventable with proper medical care during gestation, labor, and delivery.
Where the Apgar Score Falls Short
How Apgar Scores Can Impact My Birth Injury Claim
Your child’s Apgar score is part of their medical record. Low scores can support birth injury claims. For example, low Apgar scores frequently occur in babies with hypoxic-ischemic encephalopathy (HIE), a type of brain damage caused by poor oxygenation. HIE may lead to developmental or neurological conditions, such as epilepsy and cerebral palsy. Common causes of HIE include:
- Abnormal maternal blood pressure
- Fetal heart problems
- Injury to the placenta or uterus
- Complications during labor and delivery
- Poor oxygen delivery to the brain during pregnancy or birth
- Traumatic injury
- Fetal strokes
If your medical care team injured your baby by failing to uphold the medical standard of care, a low Apgar score may support a medical malpractice claim. Further, even if your injured child’s score was relatively high, don’t give up the fight. Apgar scores are just one measure of a newborn’s well-being and are far from foolproof.
Explore Your Options With a Free Consultation
Your child’s Apgar score is part of their medical record. Low scores can support birth injury claims. For example, low Apgar scores frequently occur in babies with hypoxic-ischemic encephalopathy (HIE), a type of brain damage caused by poor oxygenation. HIE may lead to developmental or neurological conditions, such as epilepsy and cerebral palsy. Common causes of HIE include:
- Abnormal maternal blood pressure
- Fetal heart problems
- Injury to the placenta or uterus
- Complications during labor and delivery
- Poor oxygen delivery to the brain during pregnancy or birth
- Traumatic injury
- Fetal strokes
If your medical care team injured your baby by failing to uphold the medical standard of care, a low Apgar score may support a medical malpractice claim. Further, even if your injured child’s score was relatively high, don’t give up the fight. Apgar scores are just one measure of a newborn’s well-being and are far from foolproof.
Sources
- Aliyu, I., Lawal, T., & Onankpa, B. (2018). Hypoxic-ischemic encephalopathy and the Apgar scoring system: The experience in a resource-limited setting. Journal of Clinical Sciences, 15(1), 18.
- Campelloni, J., & Wojcik, S. (Eds.). (2022, May 21). Neonatal hypoxic-ischemic encephalopathy. Nationwide Children’s Hospital.
- The American College of Obstetricians and Gynecologists. (2015, October). The Apgar score. ACOG.
- Lungameni, J., Maano Nghitanwa, E., & Uusiku, L. (2023). Neonatal factors associated with immediate low Apgar score in newborn babies in an intermediate hospital in Namibia: A case control study. African Health Sciences, 23(3).
- Obsa, M. S., Shanka, G. M., Menchamo, M. W., Fite, R. O., & Awol, M. A. (2020). Factors associated with Apgar score among newborns delivered by cesarean sections at Gandhi Memorial Hospital, Addis Ababa. Journal of Pregnancy, 2020, 1–6.
- Razaz, N., Cnattingius, S., & Joseph, K. (2019). Association between Apgar scores of 7 to 9 and neonatal mortality and morbidity: Population based cohort study of term infants in Sweden. BMJ, l1656.
- Simon, L. V., Hashimi, M. F., & Bragg, B. N. (2023, May 22). Apgar score. StatPearls [Internet].
- U.S. National Library of Medicine. (2022, October 22). Apgar score: Medlineplus medical encyclopedia. MedlinePlus.
- Weinberger, B., Anwar, M., Hegyi, T., Hiatt, M., Koons, A., & Paneth, N. (2000). Antecedents and neonatal consequences of low Apgar scores in preterm newborns. Archives of Pediatrics & Adolescent Medicine, 154(3), 294.